This article was written by Chance Sherer and Nikolaus Melder of VMG Health.
For each of the past five years, VMG has distributed the Intellimarker: Ambulatory Surgical Center Financial & Operations Benchmarking Study (the "Intellimarker") that compiles the financial and operational data for over 240 ASCs nationwide. A trend observed in the Intellimarker is an increase in median net revenue per case for ambulatory surgery centers for three of the last four years:
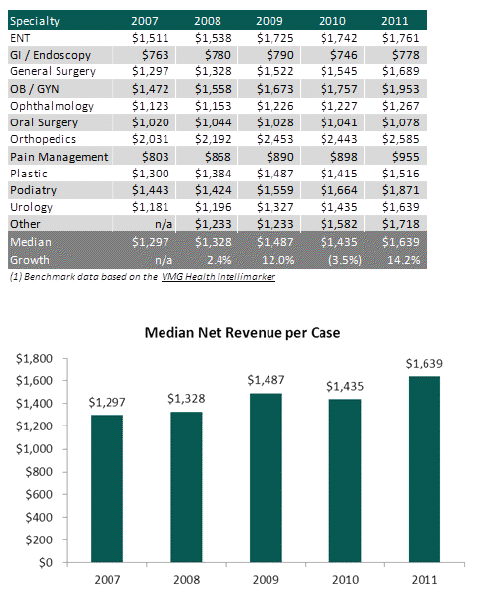
It's common to hear several industry leaders discuss both commercial and government reimbursement cuts. Surprisingly, the charts above show that the median net revenue per case (across all specialties) has increased by approximately 6.0 percent compounded annually from $1,297 in 2007 to $1,639 in 2011.
Based on discussions with management companies and administrators, there are several plausible reasons for the increase in median net revenue per case. First, the uptick in reimbursement may be explained by procedure acuity. As physicians continue to perform lower acuity procedures in-office, the number of higher acuity procedures performed in ASCs has increased.
In addition to the shift of lower acuity procedures being performed in physician offices, some procedures historically reserved for inpatient venues are now being performed in outpatient settings. This is largely due to the development of technology and the increased acumen of physicians and support staff.
Furthermore, physician-owned ASCs continue to partner with management companies and hospitals. By allowing third party management contracts and by selling their interests in ASCs to hospitals and management companies, physicians are able to mitigate financial risk and increase their ASC's billing and clinical expertise. Management companies are leveraging their knowledge and experience to negotiate optimal payment rates from commercial payors. Likewise, hospitals often leverage their current contracts with commercial payors to negotiate more favorable rates.
Another cause of the increase in net revenue per case is management's increased negotiating effectiveness. To combat increasing costs and payor pressures, ASC managers are focusing on commercial reimbursement. Many ASCs have established on-going payor contract review processes to compare rates among different payors and re-negotiate or cancel contracts.
In addition to partnering with hospitals and strengthening negotiating power, ASC managers continue to implement comprehensive ongoing reviews of their ASCs' pricing strategy. Management is utilizing current and prospective patients, surgeons, consultants, management companies, and hospital partners as sources of information to set pricing levels at optimal levels in the given marketplace.
Proactively managed ASCs continue to look for ways to remain financially, operationally, and strategically competitive. As ASCs face a mature market, it can be expected that ASC managers and administrators will continue to attempt to increase revenue as it relates to price. Given the uncertainty in future reimbursement from Medicare and commercial payors due to myriad of factors, only time will tell if these trends will continue into the future.
Learn more about VMG Health.
Related Articles on Transactions & Valuation:
Ambulatory Services of America Purchases Six Los Angeles Dialysis Centers
Medical Facilities Corporation Adds Marilynn Day-Linton to Board of Directors
NVISION Laser Eye Centers Acquires Two California Surgery Centers
For each of the past five years, VMG has distributed the Intellimarker: Ambulatory Surgical Center Financial & Operations Benchmarking Study (the "Intellimarker") that compiles the financial and operational data for over 240 ASCs nationwide. A trend observed in the Intellimarker is an increase in median net revenue per case for ambulatory surgery centers for three of the last four years:

It's common to hear several industry leaders discuss both commercial and government reimbursement cuts. Surprisingly, the charts above show that the median net revenue per case (across all specialties) has increased by approximately 6.0 percent compounded annually from $1,297 in 2007 to $1,639 in 2011.
Based on discussions with management companies and administrators, there are several plausible reasons for the increase in median net revenue per case. First, the uptick in reimbursement may be explained by procedure acuity. As physicians continue to perform lower acuity procedures in-office, the number of higher acuity procedures performed in ASCs has increased.
In addition to the shift of lower acuity procedures being performed in physician offices, some procedures historically reserved for inpatient venues are now being performed in outpatient settings. This is largely due to the development of technology and the increased acumen of physicians and support staff.
Furthermore, physician-owned ASCs continue to partner with management companies and hospitals. By allowing third party management contracts and by selling their interests in ASCs to hospitals and management companies, physicians are able to mitigate financial risk and increase their ASC's billing and clinical expertise. Management companies are leveraging their knowledge and experience to negotiate optimal payment rates from commercial payors. Likewise, hospitals often leverage their current contracts with commercial payors to negotiate more favorable rates.
Another cause of the increase in net revenue per case is management's increased negotiating effectiveness. To combat increasing costs and payor pressures, ASC managers are focusing on commercial reimbursement. Many ASCs have established on-going payor contract review processes to compare rates among different payors and re-negotiate or cancel contracts.
In addition to partnering with hospitals and strengthening negotiating power, ASC managers continue to implement comprehensive ongoing reviews of their ASCs' pricing strategy. Management is utilizing current and prospective patients, surgeons, consultants, management companies, and hospital partners as sources of information to set pricing levels at optimal levels in the given marketplace.
Proactively managed ASCs continue to look for ways to remain financially, operationally, and strategically competitive. As ASCs face a mature market, it can be expected that ASC managers and administrators will continue to attempt to increase revenue as it relates to price. Given the uncertainty in future reimbursement from Medicare and commercial payors due to myriad of factors, only time will tell if these trends will continue into the future.
Learn more about VMG Health.
Related Articles on Transactions & Valuation:
Ambulatory Services of America Purchases Six Los Angeles Dialysis Centers
Medical Facilities Corporation Adds Marilynn Day-Linton to Board of Directors
NVISION Laser Eye Centers Acquires Two California Surgery Centers

